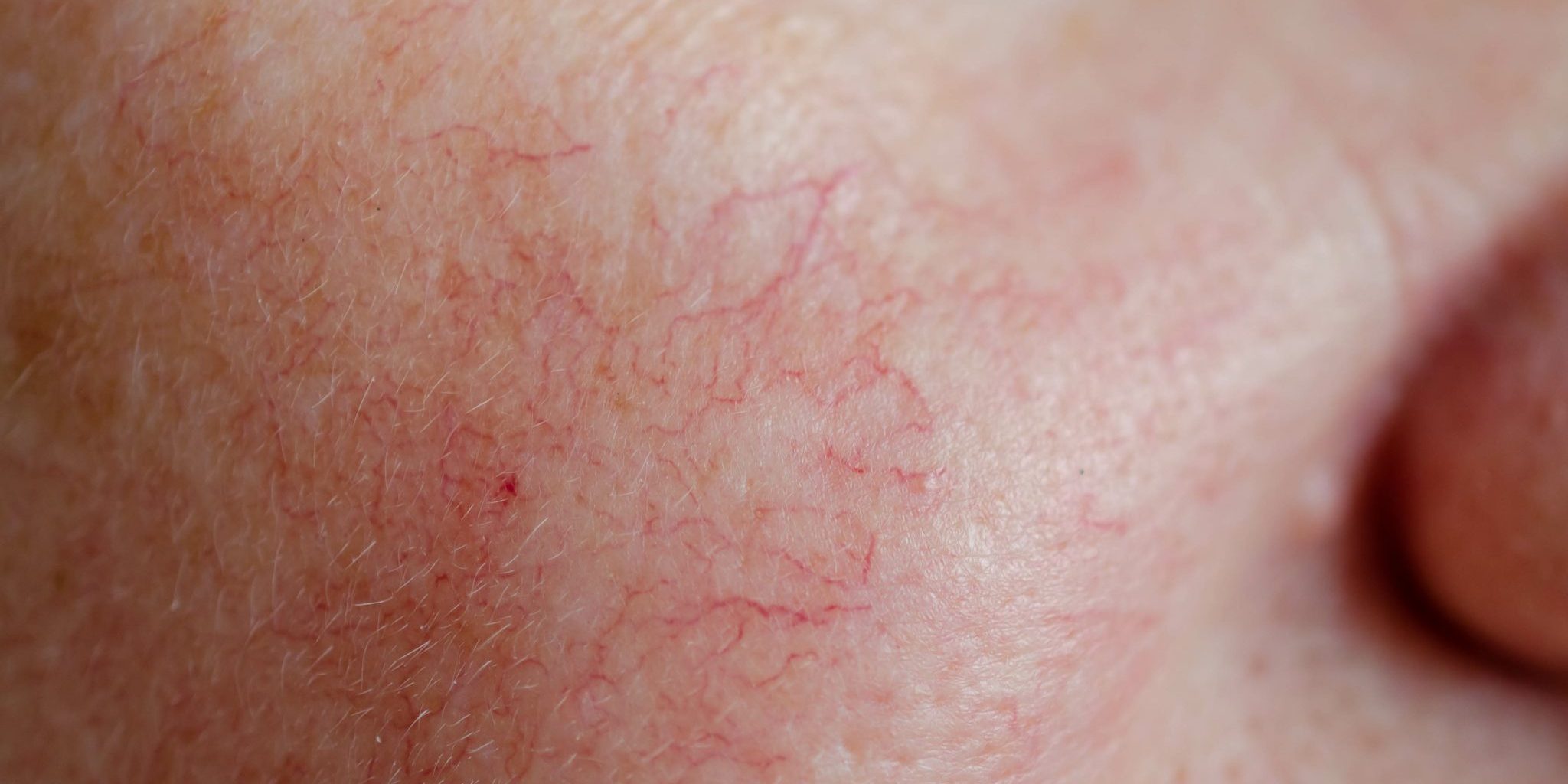
Do you suffer from broken-looking blood vessels on the nose, cheeks, and chest or anywhere on the body? These are referred to as spider veins, telangiectasia, and dilated capillaries and often develop with age. They are caused by damaged fibers that can no longer support underlying vessels, causing vessel dilation. These dilated vessels coil toward the skin’s surface, where they are visible as red, purple, or blue lines. They can be exacerbated by health issues, obesity, hormones, alcohol, and sun damage.
If you have matted telangiectasia, you see clusters of small, dilated blood vessels forming a pinkish patch on the skin. These veins are generally not harmful but can be a feature of certain autoimmune diseases affecting the skin and other connective tissues. They can also be a source of skin irritation and cause self-esteem problems.
Causes of Telangiectasia
There are different causes of telangiectasia, but pregnant women and those with the following conditions are at the most risk of developing telangiectasia.
Rosacea
Liver disease
Chronic systemic or topical corticosteroid use
Alcoholism
Scleroderma
Dermatomyositis
Lupus
Environmental factors
Genetics
Lack of exercise
Obesity
Telangiectasia can also be associated with chronic connective tissue diseases. These diseases include:
Scleroderma
Limited scleroderma or CREST syndrome (Calcinosis, Raynaud’s phenomenon, Esophageal dysmotility, Sclerosis, and Telangiectasis) affects the face, hands, and feet.
Diffuse scleroderma can affect internal organs plus the skin.
Dermatomyositis
Those with dermatomyositis find telangiectasias in sun-exposed areas of the skin, such as the V-shaped areas of the neck and chest, over the shoulder, arms, and upper back. They can be associated with brown discoloration and thinning of the skin.
Lupus
Telangiectasis of the nail folds can occur in those with lupus and Raynaud’s phenomenon. Telangiectasis can also be found on the edge of lesions on the skin and face lesions.
What should you do if you have these vein symptoms? Consult a skin care specialist or dermatologist. Symptoms can be an indication of your internal health.
Treatments for Telangiectasia
Telangiectasia itself commonly poses no health risks. However, available treatments aim to improve the skin’s appearance for health and aesthetics. You can treat telangiectasia by removing a damaged blood vessel, covering it up, or by considering some of these treatments:
Cosmetic Camouflage
Cosmetic Camouflage involves using topical creams or powders to conceal conspicuous skin conditions like telangiectasia. Use flesh tone cover-up, and you will immediately hide mild telangiectasia. For more difficult telangiectasia facial redness, use a slightly green tinted foundation or moisturizer to neutralize the color.
Sclerotherapy
Sclerotherapy is a treatment that minimizes inflammation by injecting the offending vessel with an effective sclerosing agent. A small needle is inserted into the vein, the solution is injected, and the vein collapses and disappears. Sclerotherapy treatment of telangiectatic veins is a safe and effective treatment. But there are a few side effects and some downtime.
Laser Therapy
Laser therapy is highly effective and has minimal downtime. The therapy uses a specific wavelength of light to heat hemoglobin or the protein responsible for the red color of blood. Using a state-of-the-art laser, the Fotona Nd: YAG, laser energy targets the vessels, and the heat directed at them destroys the vessels without harming the skin. Often veins treated with laser therapy can disappear almost immediately.
Electrodesiccation
Electrodessication is the insertion of a fine needle in the blood vessel. Electrical currents are then applied, and the vessel is sealed. The treatment is helpful for simple facial telangiectasia but has a scarring risk.
How to Prevent Telangiectasia
There are several ways to avoid telangiectasia and the broken blood vessels it causes. Stay away from activities that trigger flushing or facial redness and avoid these triggers:
Sunlight
Heat
Cold
Strong winds
Alcohol consumption
Smoking
Hot drinks and foods
Spicy foods
Abrasive skin cleansers
Remember to protect your skin from the sun by applying a mineral-based sunscreen with an SPF count of 30 or higher, sunglasses, and a hat. Use mild cleansers on your skin and make sure cleansers are dye or fragrance-free. Try minimizing your exposure to extreme hot or cold temperatures and avoid using topical steroids.
Contact SkinVolution Laser & Vein Center at https://skinvolutionaz.com or call us at 623-244-1902 for more information about telangiectasia, its causes, cures, and prevention.ast